Dr Jim Duff and Dr Peter Gormly take you through how to deal with ligament, muscle and tendon injuries
Sprains
Symptoms and signs
The joint is swollen, tender and painful (always compare the injured limb with the uninjured side). Gently examine for any localised very tender point and/or crepitus, both of which suggest a broken bone and therefore a complicated injury. Examine the bones above, below and around the injury.
The following tests should be done to determine the severity of the injury and exclude broken bones:
- Weight bearing/stressing the joint: the victim applies a steady force along the long bones (for ankle/ knee, ask the victim to stand; for wrist, have them place their fists against each other on their chest and push hard). Stop if pain occurs and treat as a complicated injury/ broken bone. Repeat this test at 48 hours and if weight bearing is now possible, test passive movement.
- Passive movement (you move their joint): only do this if weight bearing is possible. Test for full range in all directions (compare with other limb). A sprain will have full movement restricted in one direction by pain. If movement is restricted in two directions or more, treat as a broken bone.
Strains
Symptoms and signs
- The muscle is swollen and there may be muscle spasm. Stiffness and pain limit movement.
- A large swelling due to internal bleeding (haematoma) may appear.
- External bruising may appear, sometimes days later or far from the injury (as blood seeps internally).
General management of sprains and strains
To reduce bleeding and swelling at the injury site:
- As soon as possible, treat with rest, compression, elevation and cold treatment.
- Give painkillers.
- When pain settles, start regular non-weight bearing movements of the joint through their full range.
- Do not apply heat. Do not rub or massage the injured part. Avoid alcohol. Treating sprains and strains
- Rest: there should be no joint movement for two hours after the injury and splint applied.
- Compression: as soon as possible apply a fi rm elastic bandage to control swelling. (Stretch the bandage when making one half
of the turn, and continue without stretch for the other half. Include the fingers or toes but leave enough exposed to check circulation, sensation and movement). This reduces swelling and speeds recovery. - Elevate the injured limb above chest level.
- Cold treatment: apply cold compresses (20 minutes on, 20 off) or ice wrapped up in a towel (for just 15 minutes every hour), up to 6 treatments in the first 24 hours or until swelling has stopped.
- Stabilise the sprain with a light splint until more definitive treatment is in place (see specific sprains).
Specific sprains and strains
Ankle
An ankle sprain is usually caused by ‘going over on it’, typically to the outside.
Immediately after the injury it swells, is painful, the foot and toes tend to drop, and walking (more than four steps) is difficult or impossible.
Specific treatment:
- Strapping will be needed once the swelling is going down and the victim starts walking.
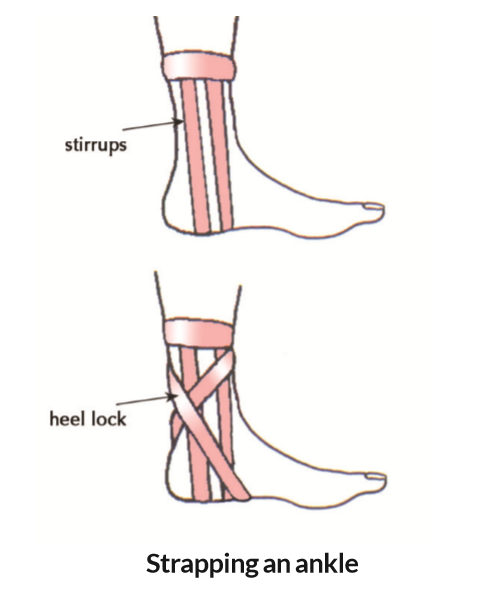
- Shave, clean and dry the lower leg and paint with tincture of benzoin to help your ‘stirrups’ (see left) stick.
- With the victim sitting, leg straight out in front of them, ask them to keep their foot from dropping by putting a loop of bandage around the toes and pulling gently to hold their foot up.
- Apply ‘stirrups’ of tape starting on the side away from the injury, down one side of the leg, under the heel and up the other side (tilt the ankle joint to the injured side as you do so to gain maximum support from the strapping).
- Hold the ends of the stirrups in place with a spiral of tape (the spiral prevents constriction of the calf).
- Apply a U-shape piece of foam mat around the anklebone (malleolus) on the injured side to control further swelling.
- Apply a pressure bandage over the strapping from toes to knee.
- Exercise the thigh (leg raises to front and back, sets of 50, 4 times daily minimum) until walking.
- Once walking, add heel locks over the strapping (these prevent re-injury).
- Strapping is left in place for one to three weeks.
Wrist
If the injury is more than minor, treat as for broken wrist.
Knee
If the knee is very swollen, suspect a more serious injury to the cartilage, ligaments, or bones. A torn cartilage may ‘lock’ the knee so that it cannot be fully straightened.
If one of the internal ligaments is torn or a knee bone broken, internal bleeding with immediate dramatic swelling of the joint will occur. Specific treatment If the injury is minor, bandage it or use an elastic knee support.
In more serious injuries:
- Straighten the knee as much as possible (stop if pain occurs/ increases)
- wrap a thick layer of cotton wool (or other soft padding) around the leg from mid-calf to mid-thigh and hold in place with wide elastic or crepe bandages. Finish off with another layer of padding and bandages, or use a well padded foam or an inflatable mattress (Thermarest™) splint.
- The victim should exercise their thigh as described for ankle, above, until walking.
- Start weight bearing when swelling and pain settle.
Trekker’s knee
The knee becomes hot, swollen and painful without any specific history of injury or fever.
This is due to exercising over several days and commonly occurs after a long descent.
Specific treatment:
- If severe, stop walking for a day or two, but bend the knee regularly (non-weight bearing).
- Apply anti-inflammatory cream and/or give painkillers (maximum dose of ibuprofen or naproxen).
- Once walking, apply adhesive tape to the kneecap so that it is pulled slightly across toward the other knee.
- Warm up the joint before setting off to walk. Use a walking stick and avoid carrying any extra weight.
Back and neck
Backs and necks can become acutely painful due to a strain, old injuries or a cold environment.
Specific treatment:
- Keep moving (although total bed rest may be needed for a day or two), keep warm and encourage good posture. Avoid positions and activities that make the pain worse.
- Relax muscle spasm with gentle massage, liniment and local heat (improvise heat pack/hot water bottle).
- Give painkillers (maximum dose of ibuprofen, with paracetamol or codeine if needed).
- Diazepam (2.5mg 8 to 12-hourly) is useful for severe muscle spasm. Sciatica (back pain extending into a leg) When a branch of the sciatic nerve is ‘trapped’ in the lower back, pain may extend (usually down one side) into a buttock, groin, down the leg or even the foot.
- There may also be ‘pins and needles’, numbness or weakness. All these signs and symptoms are made worse by moving, coughing or lifting. Treat as for back sprain, but evacuate if persistent numbness or muscle weakness occurs








